ICSI (Intracytoplasmic Sperm Injection) is an assisted reproductive technology that involves In Vitro Fertilization, often referred to as “test tube babies.” It was developed to address challenges where conventional IVF (In Vitro Fertilization) techniques are not effective. For instance, ICSI is used in cases where men have a low sperm count, weak sperm motility, or other sperm-related issues. It’s also used for women with uterus-related problems, such as those who have undergone hysterectomy, have blocked fallopian tubes, are of advanced age, or have health issues such as polycystic ovary syndrome (PCOS).
The symptoms and factors mentioned all contribute to difficulties in conceiving. Intracytoplasmic Sperm Injection (ICSI) is a method that can enhance the chances of successful fertilization and pregnancy compared to other methods.
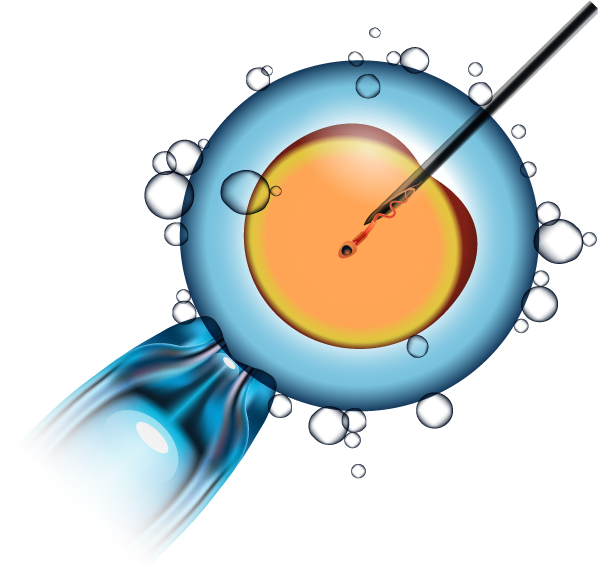

In the process of performing ICSI, scientists carefully select the healthiest and most viable egg and sperm to mix. The process is conducted by using a needle to inject the sperm directly into the egg’s cytoplasm to allow fertilization and lead to the formation of an embryo. This embryo is then transferred back into the uterus, increasing the likelihood of a successful pregnancy. ICSI significantly enhances the probability of success compared to other methods. Moreover, it offers an effective solution for couples struggling with infertility issues after attempting various other approaches without success.
Who is suitable for ICSI?
- Couples who have not achieved natural pregnancy success (difficulty conceiving).
- Men with very weak sperm characteristics including shape, motility, and quantity.
- Men who have had a vasectomy or are born with a condition preventing sperm release, but can still obtain sperm surgically (e.g., through PESA, TESE).
- Women with both blocked fallopian tubes.
- Women with ovulation disorder.
- Individuals with genetic abnormalities.
- Couples who have previously not succeeded with traditional IVF methods.
- Couples wanting genetic screening using NGS.
How to induce eggs to get large, high-quality eggs for ICSI?


For infertility treatment, what are some conditions that require Intrauterine Insemination (ICSI) for treatment?
The main purpose of ICSI is to address male infertility issues. If a couple wishes to have a child and the man is infertile, ICSI is the solution.
Currently, this technology is widely used to aid fertility in various situations, such as:
- Men who have been infertile since birth or due to vasectomy.
- Older couples, both men and women, who want to have children.
- Women with PCOS, which includes symptoms like irregular menstrual cycles or anovulation. Since there is no ovulation, pregnancy cannot occur.
- Chocolate cyst, where treatment for chocolate cyst must be carried out first. Then, egg quality needs to be evaluated. If egg quality is good, natural conception might be possible. However, if egg quality is poor, ICSI might be used to enhance the chances of successful pregnancy.
- Chromosomal abnormalities, where if either parent has abnormal chromosomes or wishes to prevent passing abnormalities to their child, including thalassemia, which is relatively common, ICSI with NGS can be used.
Advantages of ICSI
- Being the most successful method to address infertility, offering a higher chance of successful pregnancy compared to other treatment methods.
- Reducing the risk of abnormalities in the baby (such as Down syndrome, Thalassemia, etc.).
- Being applicable for patients of all age groups, particularly women at risk of infertility issues, aged 35 and above on average.
- Assisting patients in achieving a successful pregnancy even if they are of advanced age.
- Increasing the chances of successful pregnancy for individuals who have previously undergone other unsuccessful treatments.
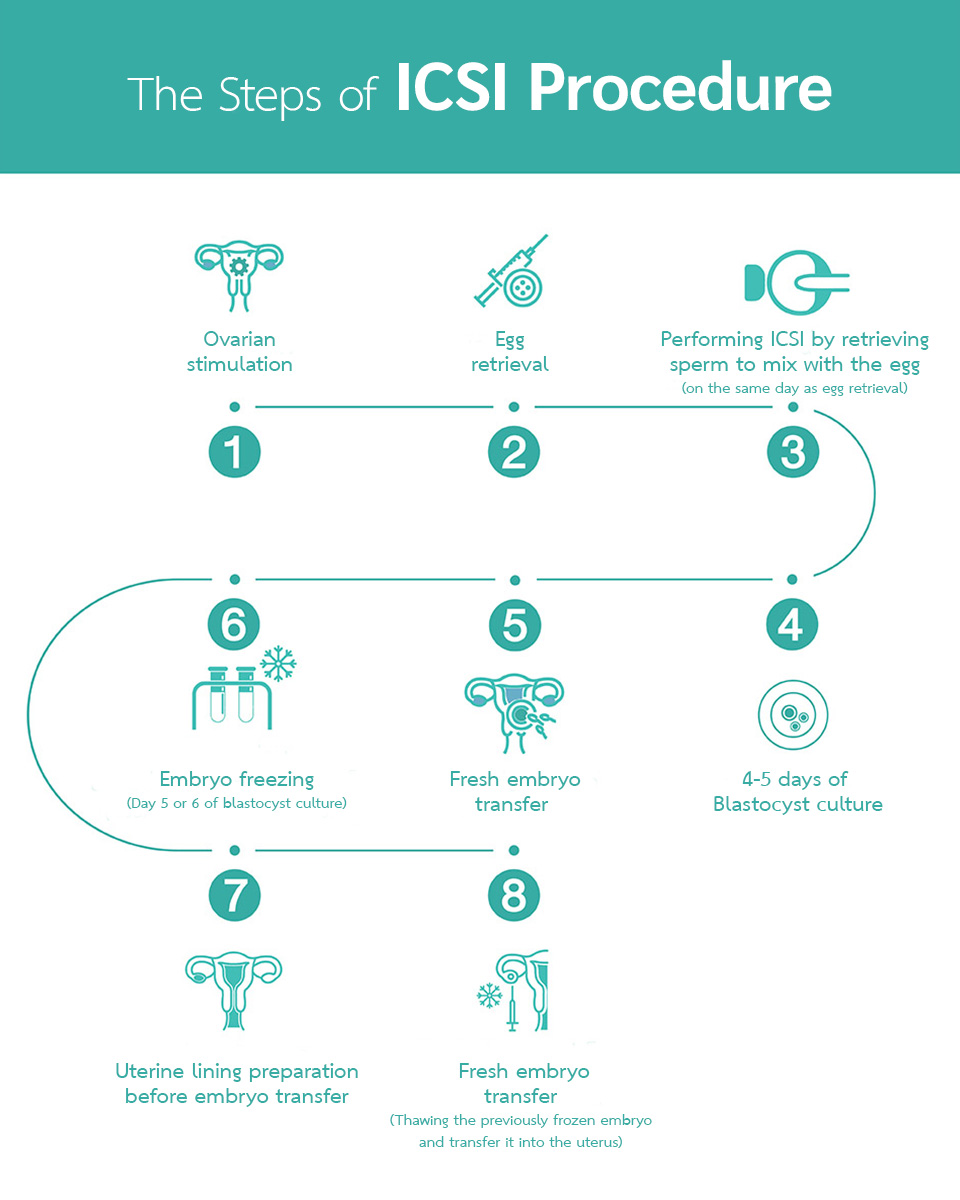
The Process of ICSI
The Making of ICSI Test Tube Babies
This method is the making of a (precise) test tube baby. It involves a new technology which is popularized worldwide. The method has been developed to address the limitations of conventional IVF and increases the chances of overcoming infertility issues in cases where the likelihood of success is low. For instance, it is beneficial for men with low sperm count, weak sperm motility, women with blocked fallopian tubes, advanced age (35 years and older), or health-related problems affecting fertility.
In the process, scientists will carefully select one mature egg and one strong and healthy sperm. This selection is performed using a microneedle to inject the sperm directly into the egg’s cytoplasm. Following this, the embryo is cultured for up to 6 days, known as Day 6, to allow for optimal development. Subsequently, the embryo is transferred back into the uterus for continued pregnancy. During the embryo transfer, the physician will determine whether to transfer the embryo at the fresh stage or after freezing.
If frozen embryo transfer is chosen, embryos are typically frozen on Day 5 – 6, though in some cases, it can be done on Day 2 – 3 based on embryo quality.
As for fresh embryo transfer, it is typically performed after the ICSI process on Day 5 – 6. However, if the embryo quality is not optimal, it may be transferred on Day 3. Moreover, to ensure a higher chance of successful treatment for infertility and to guarantee the embryo’s true completeness, “it is recommended to perform NGS Testing” alongside.
Why is Next Generation Sequencing (NGS) Necessary?
- To identify any abnormalities in embryos before implantation, reducing the likelihood of abnormalities in the baby that could lead to future miscarriages.
- To decrease the rate of miscarriages or terminations due to abnormalities in embryos.
- To achieve 100% accuracy in preimplantation genetic testing (PGT)
- To choose embryos that are robust and healthy.
- To increase the chances of successful pregnancy by 60-80%.
Who should consider genetic screening?
- Individuals who have undergone previous unsuccessful IVF attempts at IVF with unknow cause.
- Women who have experienced recurrent miscarriages.
- Women aged over 38 years.
- Women who have previously had pregnancies with chromosomal abnormalities, such as Down syndrome.

Documents required for infertility treatment with ICSI:
- National ID cards of both husband and wife.
- Marriage certificate issued by a government agency according to the law. Wedding photos cannot be used.
- certificate of name change (if any).
Why worldwide IVF


Worldwide IVF
Fertility Center by an Expert Team in ICSI And IUI Procedure with Years of Experience


High-experienced specialized doctors
Teams of specialized doctors, embryologists, and experienced nursing staff. Taking care of both Thai and foreign patients.








Medical technology and equipment
Modern and high-standard medical technology and equipment of our own to maximize success rates of pregnancy.






Expertise from many countries over the world
Consulting teams, doctors, nursing staff, and laboratory teams received training and development programs to enhance knowledge and skills, which are conducted in various countries around the world.
Doctor Profile
Dr. Thitikorn Wanichkul, M.D.
Expertise: Obstetrics-Gynecology, Gynecologic Laparoscopic Surgery, Infertility Treatment
Special Expertise: A specialized doctor in obstetrics and gynecology, further trained in gynecologic laparoscopic surgery and infertility treatment at the Chattanooga Women Laser Center and Emory University and School of Medicine in the United States. With over 20 years of experience in patient care.
Degree and institution: Doctor of Medicine (M.D.), Prince of Songkhla University, 1990
Diploma: Department of Obstetrics and Gynecology
Postgraduate Education: Reproductive Endocrinology, Emory University School of Medicine, United States, 2000-2002
Specialized Training: Advanced Laparoscopy & Laser Surgery
Original Affiliation: Phyathai 2 Hospital


Successful Case